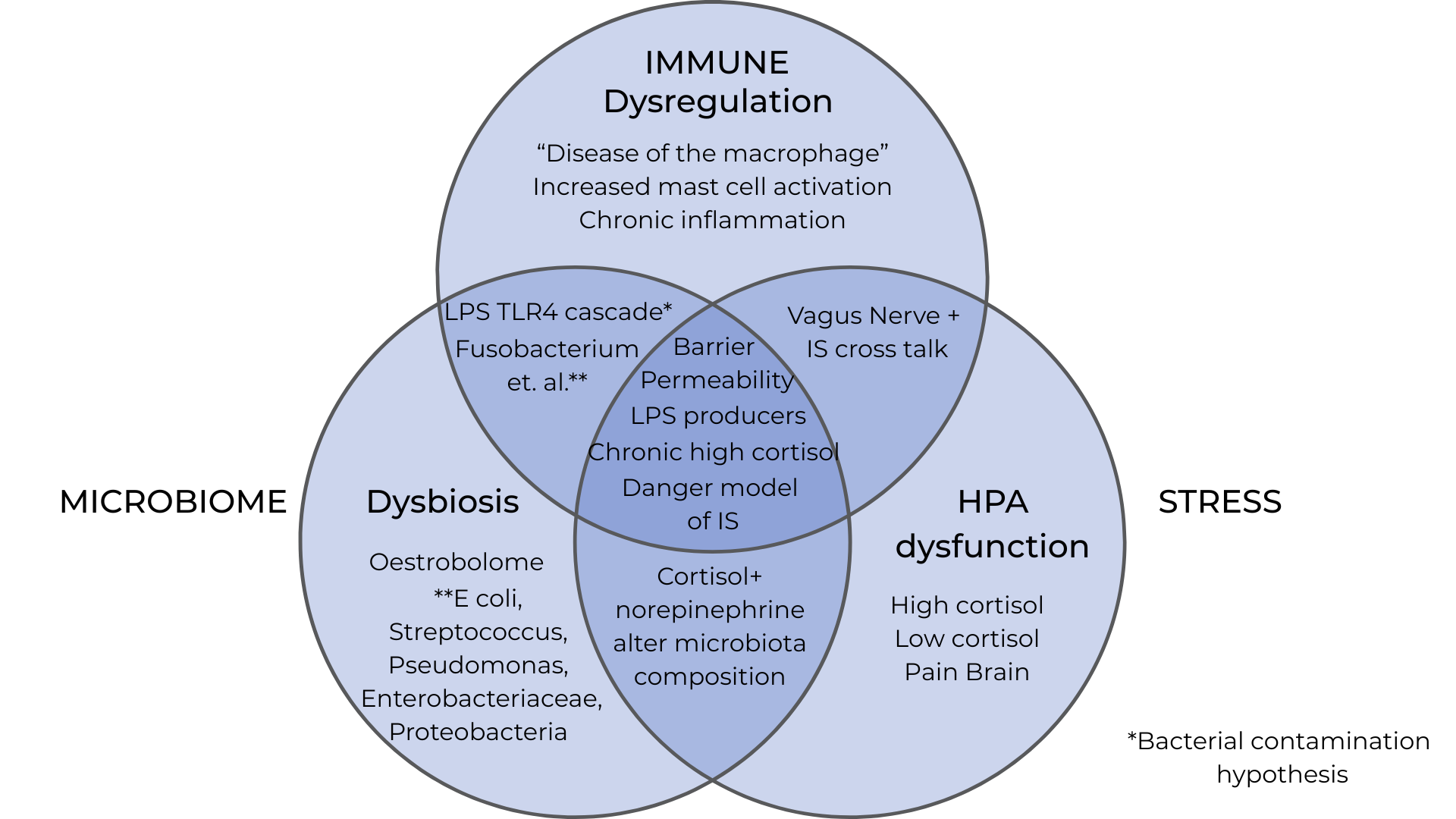
Scratching the Surface of Immune-Microbiome-Stress Connection in Endometriosis
March is Endometriosis Awareness Month. A lot of you have already heard me talk about endometriosis extensively, but, for anyone who's forgotten, it's a sysetmic inflammatory condition meaning that it can affect the whole body, and it is characterised by tissue that is similar to the uterine lining growing in other places in the body. It is predominantly found in the pelvis, but it has been found all over the body. I read something the other day about someone who had wrist surgery, and they found endometriosis-like tissue in the wrist, it's been found in the eye, it's been found in the brain so, it is possible that this tissue can metastasise.
Unfortunately, the average diagnosis time in the UK has increased to just under 9 years. Back in 2017 we were at the 7.5 year mark. As a reminder, this is the time between first mentioning symptoms to a GP and eventual diagnosis. There are multiple contributing factors here but one of the main reasons is that for decades, the gold standard of diagnosis has been surgery, which is a large hurdle to jump through. The American College of Obstetricians and Gynaecologists has just published new guidelines suggesting that clinical symptoms should be considered enough for a diagnosis, which could mean that diagnostic time drops rapidly in the US. Who knows if the UK will follow suit, I do know there are some exciting non-invasive diagnostic tools being researched that could be a complete game changer.
A lot of clients who are managing this condition, feel quite frustrated with the medical approach to it, and that's because there's still a lot of focus on only managing the hormonal side of things.
The condition is quite hormonally driven, so the tissue that's growing in places where it shouldn't be is very oestrogen sensitive, it can contribute to the growth of tissue where it shouldn’t be and the creation of a blood supple and nerves to the tissue (angiogenesis and neurogenesis) so, it is important that we manage that as best as we can, but normally we do that through making sure it's broken down healthy detoxification pathways, making sure that we have very healthy bowel movements so that we're able to get oestrogen out of the body easily, and also things like making sure that we're having enough fibre and we're stimulating bile enough. Those are some of the lifestyle things that we do to manage the hormone side of things. The endometriosis tissue creates its own oestrogen, so if the only medical intervention is to try and stunt your body’s oestrogen production, you’re missing a few options.
We’re leaving a lot of possible recommendations and symptom management on the table if we're not thinking about the immune system, the microbiome and the stress response. That's what I've been talking to practitioners about this month. So, if there's tissue growing where there shouldn't be, there is a level of immune suppression, because normally the immune system would be seeing that tissue and getting rid of it.
However, we're also seeing a lot of inflammation and pain and that is suggestive of an up-regulation of inflammation, a different immune system response. So there are some parts of the immune system that are suppressed and some that are up-regulated. We can do things like making sure that we're taking the pressure off other areas, making sure there are no underlying infections and things like that, that helps to manage the inflammatory response a little bit better.
We also need to think about the microbiome because often that is the home of possible inflammatory drivers. If we've got a lot of inflammatory bacteria there, we often have a lot of digestive symptoms. Many of us with an endometriosis diagnosis were told many years before that we have IBS. We know there's a big link between gut symptoms and endometriosis and there is a lot of interplay between the bacteria and other organisms in the gut and the immune system. The gut also has an important role in the oestrogen detoxification process and there are particular gut bacteria that can help or hinder this.
The next overlap I want to discuss is between the stress response and both the immune system and the microbiome, this isn't something that we should ignore either. A really common symptom in endometriosis is pain, not everyone with endometriosis experiences it but many do, either pelvic pain, pain with your cycle, or pain throughout the month, that can be indicative of endometriosis, and this occurrence of chronic pain is something that does influence our stress response, because our body will release cortisol to try and dampen pain, and very often when we do look into the stress response, we see either high levels of cortisol or low levels of cortisol. Now, cortisol is a bit of a Goldilocks hormone. We want the right amount, so too much is not good, and too little is not good either. It needs to be just right. Cortisol and adrenaline also influence the bacteria in the gut. We also have our Vagus nerve, the main connection between our gut and our brain as an immune system regulator, as well as being the main way our body switches between a stressed state (sympathetic response) and a non-stressed state (parasympathetic response).
All this to say, when we are approaching endometriosis from a holistic perspective, we need to consider how can we influence the immune response, the microbiome, and the stress response, so that we are able to manage the symptoms and improve our quality of life. Let me know which of these areas you’d like to know more about.